
The Clock Is Ticking on Insurance Claims Expertise — And “AI” Alone Won’t Save You
A strategic perspective on preserving institutional knowledge, upholding good faith obligations, and choosing AI that is actually built for the work.
The Retirement Wave Is a Claims Quality Problem
Most discussions about the insurance talent shortage focus on headcount. The more consequential issue is what leaves with the people. Written guidelines capture the what. The judgment developed over a career — knowing which questions reveal a fraudulent narrative, which details signal a claim is about to escalate, which coverage nuances matter for this specific loss type — that captures the how. It is that judgment, not the documentation of it, that makes consistent, good-faith claims handling possible. And it is precisely what is walking out the door.
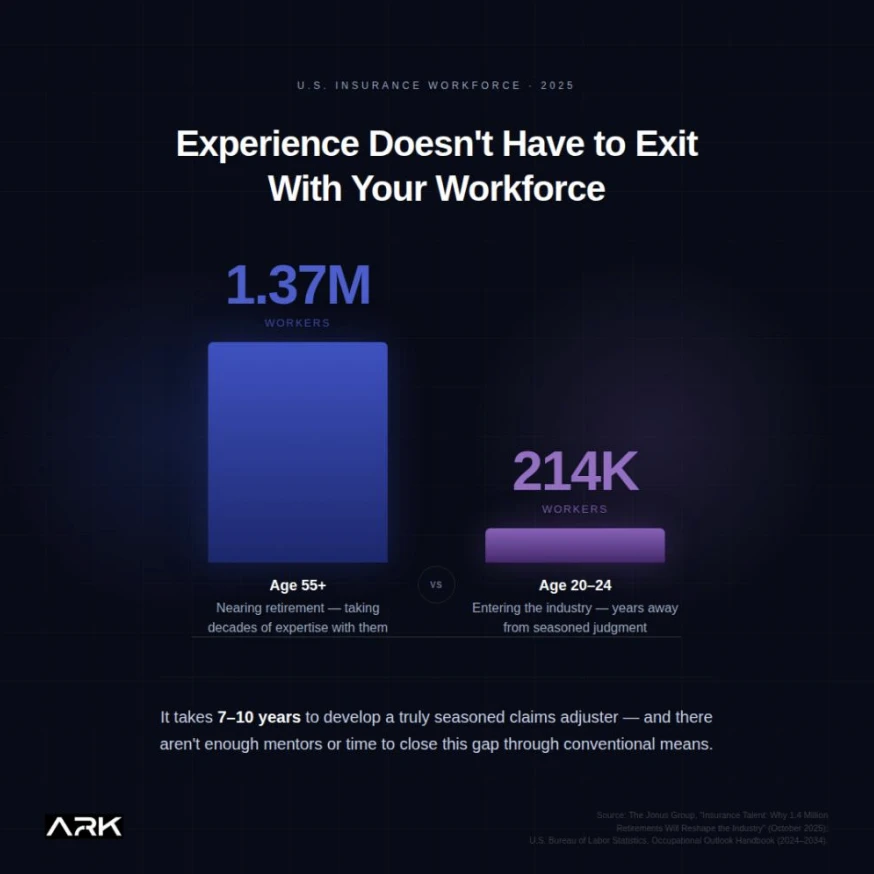
The scale is significant. Current U.S. Bureau of Labor Statistics (BLS) data shows 1.37 million insurance professionals are age 55 or older — nearly one in four workers — against only 214,000 between ages 20 and 24.[1] The industry’s median age of 44 already exceeds the national workforce median and is aging faster than peer sectors.[1] The U.S. Chamber of Commerce projects that half of the current insurance workforce will retire within 15 years, leaving more than 400,000 positions unfilled.[2] On the claims side alone, 25% of adjusters are expected to retire within five years,[2] with the BLS projecting 21,600 claims positions opening annually over the next decade — nearly all replacement, not growth.[3]
Research puts the development timeline for a truly seasoned adjuster at 7 to 10 years.[1] The industry does not have the time, the mentors, or the training infrastructure to close that gap through conventional means. The question for carrier leadership is not whether this transition will affect claims quality — it already is. The question is what you intend to do about it before the window closes.
The carriers who act in the next three to five years will preserve a standard of claims handling that their competitors, who waited, will spend years trying to rebuild.
What the Gap Costs — Beyond Headcount
The operational consequences of an undertrained claims workforce compound in ways that don’t always show up as a single line item. They show up as claim cycle times that extend. Files that require rework. Fraud that goes undetected at intake and surfaces later in litigation. Policyholders whose experience at first contact sets the tone for a relationship that either holds or doesn’t.
Adjuster retention compounds the problem. High turnover rates in claims roles — particularly in the early years of an adjuster’s career — mean carriers are not simply managing a one-time retirement transition. They are continuously cycling through an undertrained workforce that rarely reaches the depth of expertise the role requires before moving on. Each transition is a gap in coverage, knowledge, documentation discipline, and the pattern recognition that only develops through experience.
For carrier leadership, the stakes of this gap are fundamentally about the organization’s ability to meet its good faith obligations at scale — to investigate thoroughly, determine accurately, and respond promptly, regardless of who handles the claim or when it comes in. That standard doesn’t move. The workforce capable of meeting it reliably is shrinking.
The Question Isn’t Whether Your AI Is Smart — It’s Whether It Speaks Insurance
The conversation about AI in insurance has outpaced the reality of what most AI tools are actually built to do. Carriers are being offered automation — workflow tools, chatbots, intake platforms — presented as solutions to a problem that continues to evolve and is fundamentally about knowledge, judgment, and consistency. At the pace AI is advancing, purpose-built solutions grow with your business — and with the industry.
The right AI doesn’t arrive knowing your business — it’s built to learn it, retain it, and continue growing with it. That’s the difference between a tool that solves one problem today and a solution that serves your organization for the long term. The intake approach your best adjusters have refined over careers — that institutional knowledge doesn’t exist in any off-the-shelf tool. It exists in your organization. ARK provides the architecture to capture it, structure it, and put it to work — but the intelligence that makes it yours comes from you.
The BLS projects that AI will “continue to increase efficiency and make workers more productive” in claims — while simultaneously projecting a 5% decline in adjuster employment through 2034, even as tens of thousands of positions open each year to replace departing workers.[3] Technology will reshape the claims profession. The carriers who lead through that shift will be those who ensure their AI is built with the rigor and specificity the role demands — not those who adopt the nearest available tool and call it a strategy.
The question is not whether your organization is using AI. It is whether it is working alongside your team — capturing knowledge, handling intake thoroughly, and freeing your adjusters to focus on what retains the policyholder.
What Curated AI Does Differently
ARK builds AI Assistants for insurance carriers that are purpose-built around institutional knowledge — not deployed off the shelf, but developed in partnership with each carrier to reflect their specific lines of business, their policy language, their documentation standards, and the judgment their most experienced adjusters have developed over careers.
The distinction matters at every point in the claims workflow, but it is most consequential at FNOL — the moment that determines the quality of everything that follows.
FNOL Guided Conversationally — by Phone, Web, or Email
ARK’s AI Assistants are designed to guide policyholders through First Notice of Loss across the channels they actually use — phone, web, and email — with no hold times and no queue. At the moment a policyholder needs to report a loss, the AI is available to begin a structured, conversational intake immediately, around the clock, regardless of call volume or time of day.
The AI Assistant guides the conversation — asking questions, following up on incomplete responses, and keeping the intake moving toward a complete picture of the reported loss. It does not interpret coverage or make claims determinations. Those responsibilities remain with the licensed adjuster who receives the file. What the AI Assistant contributes is a more complete, better-organized starting point than a junior adjuster without mentorship is likely to produce on their own.
In practice, more than 90% of FNOL interactions are guided to completion without requiring escalation to a human adjuster. For those that do require human involvement, the transition is designed to be seamless — the adjuster inherits a structured record of what was discussed, so the policyholder isn’t asked to start over, and the adjuster isn’t starting from nothing.
Across modalities, ARK’s Assistants currently support up to 34 languages, with language auto-detected rather than selected — so policyholders aren’t navigating a menu before they can report their loss. For carriers serving linguistically diverse communities, the ability to guide a policyholder through FNOL in their own language, consistently and without friction, reflects a meaningful standard of accessible service.
Fraud Awareness Woven Into the Conversation
Fraud pattern recognition is among the most experience-dependent skills in claims — built over years of exposure to how loss narratives present and where the details that matter tend to be missing. It is precisely the kind of judgment that retires with tenured adjusters and is rarely transferred in time.
ARK’s AI Assistants are designed with that awareness built into the conversational flow — guided by the indicators experienced adjusters and SIU professionals have learned to recognize. When the intake conversation surfaces patterns worth noting, they are documented professionally in the file for the licensed adjuster’s review. The adjuster inherits a more informed starting point than a conventional intake would typically provide.
Built to Know When to Step Back
Questions about coverage, policy language, and claims determinations require a licensed adjuster — and ARK’s AI Assistants are deliberately designed to stay on the right side of that line. When a conversation moves toward territory that calls for licensed professional judgment, the AI is built to acknowledge the question, let the policyholder know it will be addressed by their adjuster, and transition accordingly.
This is not a limitation of the technology. It is a foundational design principle: the AI guides the intake conversation within the scope it is authorized to occupy. Anything beyond that scope belongs to the professionals whose licensure and judgment the AI exists to support, not replace.
A More Informed Starting Point for Every Adjuster
When an ARK AI Assistant guides a FNOL conversation to completion, the licensed adjuster who receives the file inherits more than a transcript. They inherit a structured record — questions asked, responses given, gaps noted, and observations documented — that reflects the intake approach encoded from the carrier’s own experienced professionals.
For a junior adjuster still building expertise, that file is also a reference point: a consistent illustration of how a thorough FNOL conversation is structured for this type of claim. Over time, that repeated exposure contributes to better professional judgment — not by replacing the learning process, but by giving it a more substantive foundation. As the Jonus Group noted in October 2025, proactive knowledge transfer paired with technology is the defining strategic choice for carriers navigating this transition.[1]
What Carrier Leadership Should Expect from This Investment
The outcomes of deploying curated AI in claims are interconnected — and they compound in the direction of organizational integrity rather than away from it:
- Claims intake guided to a higher standard: Every FNOL conversation guided with the same structured questioning and documentation approach, regardless of volume, time of day, or adjuster experience level. The licensed adjuster inherits a more complete starting point.
- Policyholder experience that reflects the carrier’s commitment: Immediate availability across modalities, no hold times, and intake support in up to 34 languages communicate responsiveness at the moment policyholders are most attentive to how their carrier shows up.
- Fraud awareness built into the conversation: Patterns and observations worth noting are documented professionally in the file for the licensed adjuster’s review — giving them a more informed starting point than a conventional intake would typically provide.
- A more informed adjuster workforce: Junior adjusters inheriting well-structured files gain a consistent reference point for what thorough intake looks like — contributing to professional development in a way that classroom training alone cannot replicate.
- A record that supports the carrier’s position: A structured, consistent account of every first contact — what was asked, what was shared, what was noted — providing a defensible record of how the intake was handled from the moment the claim was reported.
Good faith claims handling has always required thorough investigation, accurate determination, and timely response. Curated AI doesn’t change that standard — it makes meeting it consistently possible, even as the workforce that once carried it retires.
The Decision Window Is Narrowing
The Jonus Group’s October 2025 analysis identified a three-to-five year window for carriers to act before the knowledge drain becomes effectively irreversible.[1] After that point, the professionals who could teach the AI what expert-level claims handling looks like will largely be gone. What remains will be a younger, thinner base of institutional knowledge — and AI built on that foundation will reflect it.
The good faith obligations this industry operates under do not accommodate workforce transitions. The policyholder filing a claim today is entitled to the same standard of handling as the one who filed last year, when the adjuster who answered had twenty years of experience. Curated AI is how carriers honor that obligation continuously — not just when staffing allows.
Not All AI Is the Same. The Difference Is What It Was Built to Know.
The insurance industry will adopt AI. The question for carrier leadership is whether the AI your organization adopts is built with the specificity, the domain depth, and the institutional knowledge that claims handling actually requires — or whether it is a general-purpose tool dressed in insurance language.
ARK builds curated AI Assistants in partnership with carriers — trained on your institutional knowledge, calibrated to your lines of business, and built with the guardrails your regulatory environment demands. The result is not an automation layer. It is a claims capability: consistent, knowledgeable, always available, and designed to deliver the kind of customer experience and intake quality that reflects your organization at its best.
We welcome the conversation. Visit arkproject.com to learn more about what curated AI looks like in practice — and what it could mean for your organization.
ARK partners with carrier leadership to build curated AI Assistants that preserve claims expertise, uphold good faith standards, and develop the next generation of claims professionals — purpose-built for your organization, not adapted from a generic platform.
Sources
All citations are from sources published in 2025 or reflect BLS data covering the 2024–2034 projection period.
[1] The Jonus Group (October 2025) — “Insurance Talent: Why 1.4 Million Retirements Will Reshape the Industry.” Source of: 1.37M workers 55+, 214K workers 20–24, median age 44, 7–10 years to develop expertise, 3–5 year action window. Draws on U.S. Bureau of Labor Statistics workforce age data.
https://www.jonusgroup.com/blog/2025/10/insurance-talent-why-1-dot-4-million-retirements-will-reshape-the industry
[2] Hi Marley (September 9, 2025) — “How Carriers Can Survive the Insurance Talent Drain.” Source of: 50% of workforce retiring in 15 years / 400,000+ open positions (citing U.S. Chamber of Commerce); 25% of claims adjusters retiring within 5 years. https://www.himarley.com/blog/how-carriers-can-survive-the-insurance-talent drain/
[3] U.S. Bureau of Labor Statistics — Occupational Outlook Handbook (2024–2034 projection cycle) — Claims Adjusters, Appraisers, Examiners, and Investigators. Source of: 21,600 projected annual openings; 5% projected employment decline 2024–2034; AI/technology impact on productivity and role scope. https://www.bls.gov/ooh/business-and-financial/claims-adjusters-appraisers-examiners-and-investigators.htm
